Accurate staging guides management and can improve outcomes, including digit salvage.
While frozen, mild and severe frostbite may appear similar. True severity often becomes clear only after rewarming and may evolve over several days.
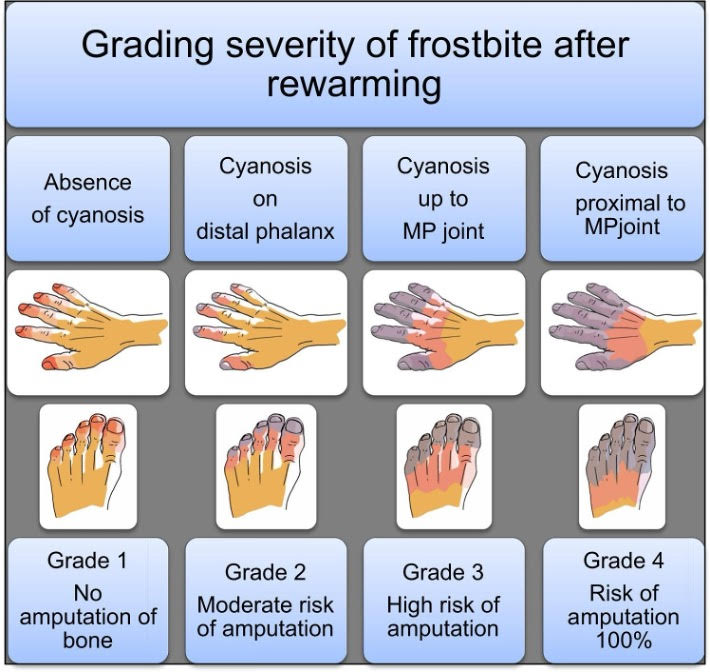
Assess severity after rewarming using the Cauchy classification.
The Cauchy classification predicts the natural course of frostbite if untreated.